How Does Cobra Insurance Work
If you become eligible for a COBRA plan, such as losing your job, the employer will contact the health insurer about the situation within 30 days of your last day.
The health insurance company will then notify you with information about how to sign up for COBRA. That information will include cost estimates, so you understand how much you have to pay to keep the health plan through COBRA.
You can sign up for COBRA coverage or decline coverage. You have 60 days to make that decision.
Once signed up for COBRA, youll use your health insurance plan like you did when employed. However, youll pay all of the costs with no help from your former employer.
You can keep COBRA for at least 18 months. In some cases, you can have a COBRA plan for even longer — up to 36 months — depending on the qualifying event.
At the end of your eligibility period, you need to find another health plan if you want insurance. Check the COBRA coverage alternatives section later on this page for other options.
Figuring Out Health Insurance
Nearly half of Americans get their health insurance through their employer. If you’ve just left your job, you’ll want to figure out how to get new coverage as soon as possible.
Most people who quit will lose their employer-sponsored health insurance at the end of the calendar month, said Laurel Lucia, director of the Health Care Program at the University of California Berkeley’s Center for Labor Research and Education.
If you don’t have another job lined up that will provide health insurance, you may be eligible for Medicaid or a subsidized plan on the Affordable Care Act’s marketplace. Medicaid typically involves no or low monthly premiums, Lucia said. And marketplace plans are the cheapest they’ve ever been for many people, thanks to relief legislation passed in the pandemic.
You can compare your options at Healthcare.gov.
More from Personal Finance:Mobile payment app complaints surge as more Americans go cashless
The Consolidated Omnibus Budget Reconciliation Act, or COBRA, allows people who work at companies with 20 or more employees to pay to continue their workplace insurance plan for certain periods of time. The option is pricey $600 a month, on average because you’re now shouldering the cost of the entire plan.
Even if you plan to start a new job soon with new insurance, these options may be worth exploring if there’s going to be any gap in your coverage .
Medicare Medicaid And Chip
If youre nearing 65 or have disabilities, and need low-cost coverage, you may want to consider Medicare and/or Medicaid. While Medicare and Medicaid are both health insurance programs administered by the government, there are differences in covered services and cost-sharing. Visit the Texas Health and Human Services website for more info on Medicaid in Texas. To learn more about Medicare, visit medicare.gov or call 1-800-633-4227.
If you have children and need free or low-cost coverage, you may want to consider the Childrens Health Insurance Program . Visit HHS website for more info on the CHIP program.
* You can apply for and enroll in Medicaid, Medicare, or CHIP any time of year.
Also Check: Is Ivf Covered By Health Insurance
A Number Of Circumstances For Quitting Are Considered Just Cause
You are justified voluntarily leaving your job in the following situations if, considering all the circumstances, quitting your job was the only reasonable alternative in your case:
Various reasons may prompt you to quit voluntarily your employment. However, to be paid list of 40 main reasons which may justify voluntarily leaving. You will find for each situation, an overview of the reason, reasonable alternatives that may be used and why the reason for quitting is considered to be with just cause.
Can You Change From Cobra To A Marketplace Plan
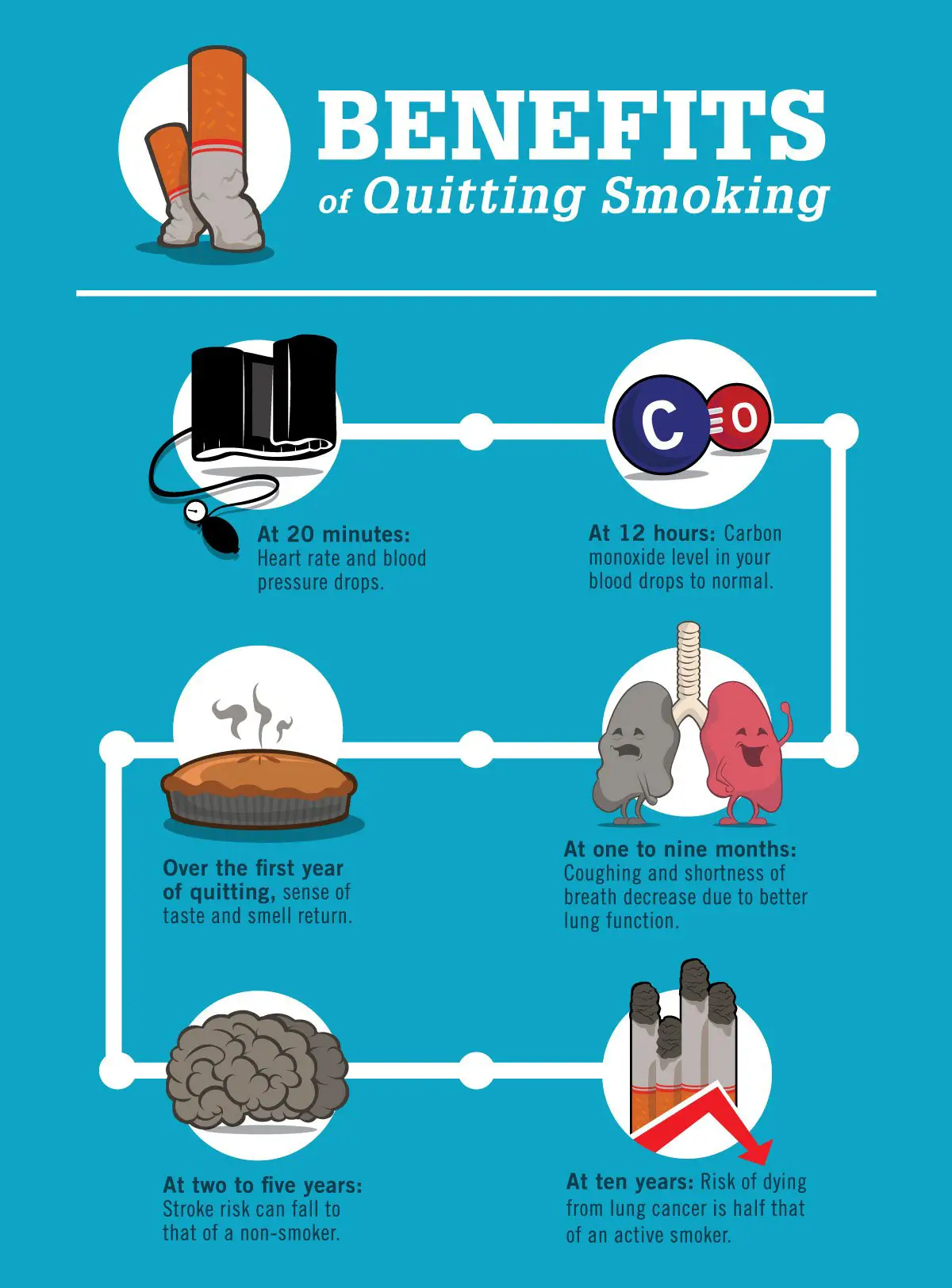
Yes, you can change from COBRA to a Marketplace plan during the open enrollment period if-
- You decide to end your COBRA plan early.
- Your COBRA insurance plan is going to expire soon.
- The amount you usually pay for COBRA changes because your former employer stopped contributing towards your health insurance plan or you lost a government subsidy, and now you will have to pay the full cost.
Also Check: How To Get Low Health Insurance
How Long Does Cobra Coverage Last
Most employees can keep COBRA coverage for 18 months after termination.
Employees, spouses and dependent children can keep it for 18 months if the employee was terminated and it wasnt for gross misconduct. Those people are also eligible if the company reduces the employees hours and the person is no longer eligible for employer-sponsored health insurance.
COBRA insurance can last longer depending on the situation. Someone with a total disability can keep it for 29 months. Also, other instances can allow people to keep COBRA for 36 months. These situations include covering a spouse after the employees death, a divorce or legal separation and a dependent child who loses coverage.
What Happens To Insurance When You Get Fired Or Quit
Typically, your health insurance coverage will automatically stop when you cease your employment. The specific details may vary based on your company policies, so you should discuss this matter with your human resources manager. Some companies may allow you to benefit from this coverage until the last day of the month that you quit. For others, your health insurance may end the day after you get fired or laid off.
The good news is that you can typically take advantage of a special federal law under the Consolidated Omnibus Budget Reconciliation Act, or COBRA. This law allows employees to continue taking advantage of their employer-provided health insurance whether they were laid off, fired, or quit. Workers are also eligible for COBRA benefits if the employer reduces their hours below a minimum threshold.
You May Like: How To Get Travel Health Insurance
Pay Cobra Premiums Using Your Health Savings Account
If youre losing your health insurance as a result of leaving your job, you can use the money in your HSA to pay the monthly premiums for COBRA continuation of your health insurance. This is considered a qualified medical expense, so you wont have to pay income taxes on the withdrawals, and you won’t be subject to the 20% penalty that applies to HSA withdrawals that aren’t used for qualified medical expenses.
What if you cant afford COBRA, dont want to continue your current health plan, or arent eligible for COBRA? As long as youre receiving federal or state unemployment benefits, you may withdraw the money in your HSA to pay health insurance premiums. For example, you could purchase a health plan from your states Affordable Care Act health insurance exchange and use money from your HSA to pay the premiums. Depending on your income, you may even be eligible for a government subsidy to help you pay the monthly premiums so your HSA funds stretch further.
But once you’re no longer receiving unemployment benefits, you cannot use pre-tax HSA funds to pay your health insurance premiums .
As soon as you stop receiving unemployment benefits, don’t forget to stop using your HSA funds to pay those health insurance premiums.
Is Cobra Insurance Right For You
COBRA may be a wise decision if you want to make sure your providers are in the network and you cant find a more affordable plan that they take.
COBRA coverage may also be good if you expect to get another health insurance plan soon and want to make sure you have comprehensive health insurance for a limited time.
Also Check: When An Insurer Issues An Individual Health Insurance Policy
Employee Benefits When You Leave Your Job
Have you recently left your job, or are you about to move on? Whether you quit or were terminated, you may be entitled to certain employee benefits.
It pays to learn as much as you can about these benefits before you move on to something new. In many cases, its harder to learn about your rights when youve already turned in your lanyard or equipment and lost your face-to-face access to HR.
If You Lose Your Job You May Have The Right To Continue Your Health Insurance Coverage For 18 Monthsbut You’ll Have To Pay The Full Premium
The Consolidated Omnibus Budget Reconciliation Act, known as COBRA, is a federal law that allows employees to continue their employer-provided health insurance after they are laid off or fired, or they otherwise become ineligible for benefits . The employee has to pay the full premium at the employer-negotiated group rate, which is typically less expensive than it would be to buy an individual policy on the open market.
Read Also: Do You Have To Have Health Insurance To File Taxes
Pros And Cons Of Cobra
Pros:
- COBRA continuation coverage is a great option for individuals who change their employment situation. It allows them to continue health insurance on the same group plan.
- It is an effective way to keep your health insurance until you qualify for another plan.
- You can continue using the same methods for filing claims, doctors, and pharmacists that you used before.
- With COBRA, you can save money on out-of-pocket costs.
- A COBRA beneficiary might be able to get help from public assistance programs like Medicaid or other state or local programs.
Cons:
- COBRA insurance plans have high premiums.
- If your employer changes the health plan coverage, your coverage will change under COBRA.
- You can stay on a COBRA plan for only 18-36 months.
- If you are using COBRA to continue your health insurance, some companies will charge you an additional 2% on top of your premium.
What About Your Meds
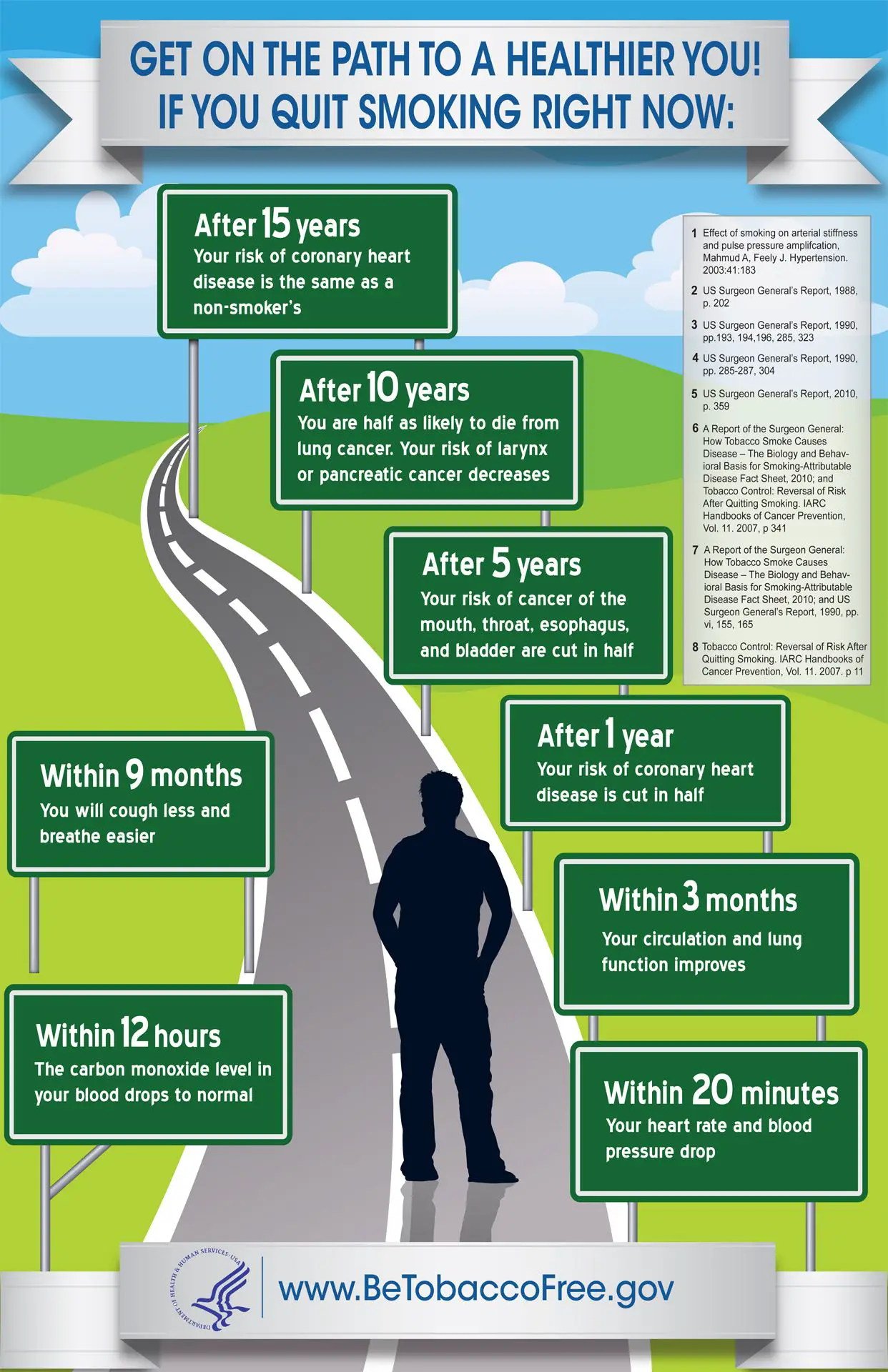
One important health issue anyone should consider before quitting: prescription medications.
“If a person is on a chronic illness prescription drug, they do not want to mess around without insurance,â Millen says. âThese drugs can be very expensive without insurance. Insulin, for instance, is a life-saving drug.â
You may want to stock up if your plan allows it.
âIf you have an ongoing prescription during a time of not having health insurance, I would recommend getting multiple months filled before you know youâre going to quit your job,â DiNardo says.
âMail-order prescriptions are typically less than the cost of regular monthly fills,â she points out. âYou could also speak to your doctor and find out if thereâs a generic version of the drug that would be more affordable for you while you are without insurance coverage.â
Don’t Miss: Can You Add Spouse To Health Insurance
If I Drop Cobra Coverage During The Election Period Can I Get It Back On A Later Date
If you waive COBRA coverage, you can revoke the waiver later — as long as you’re still within the 60-day election period. The coverage is retroactive to when you became eligible for COBRA, as long as you pay the premiums retroactively.
You can also cancel COBRA coverage at any time — you’re not locked into an 18-month commitment when you sign up.
COBRA coverage ends when you:
- Reach the end of your coverage period
- Stop paying premiums
COBRA coverage also ends if the employer:
- Goes out of business
- Stops offering health insurance benefits to workers
If the employer changes health plans, you can switch to the new plan like everybody else, but you can’t keep the old plan in that case.
COBRA applies to private-sector companies with 20 or more employees as well as state and local governments. Some states also have “mini-COBRA” laws that apply to employers with fewer than 20 workers. See the section below for more information about mini-COBRA plans.
If you have a family health plan, not all family members have to enroll in COBRA. For instance, you can waive the option, but your spouse and kids could still elect COBRA, or vice versa.
Before You Choose A Short
When it comes to health insurance, its very important to know what youll be getting into ahead of time. Short-term health insurance plans arent sold in the ACA Marketplace, and therefore often do not follow the standards of a typical ACA health insurance plan. This means that providers of short-term health insurance can put a lot of limits on their plans that are typically not allowed on an ACA plan. Some of these limits include:
- Eligibility based on your health status. Applicants for short-term health insurance policies will typically be asked questions about their health and may deny coverage to those who answer yes to these questions. For example, if you are asked whether or not you have a serious pre-existing condition* and you answer yes, then you will likely be denied coverage based on your condition.
- Renewability of your short-term plan. With a short-term health insurance plan, your coverage ends once your policy term is up. While some of these types of policies include an option to extend or renew coverage, most do not**.
- Limits on benefits covered by your plan. Short-term health insurance policies can put a variety of limits on benefits covered by a plan, from covered doctor visits to prescription drug coverage***.
Recommended Reading: How To Get The Most Out Of My Health Insurance
How Does Group Health Insurance Work Between Jobs
Typically, the Group Insurance Scheme provided by your employer ends on the last working day of the employee. However, some companies in the country provide group insurance coverage for employees and pay the premium in full or partially. However, can the group insurance cover be transferred or converted to an individual health insurance policy in case you want to change jobs, or you have been laid off?
The Insurance Regulatory and Development Authority of India states that an employee can convert the group cover to an individual health insurance plan with the same insurance company after completing the required formalities.
That being said, the insurance provider has the full right to decide on the terms and conditions of the new policy. This option of switching from group insurance to individual insurance is offered only by a few insurance companies and employers. Hence, you need to check with your employer if there is an option to remain with the same insurer, except that it will be converted to an individual insurance plan.
You may have to pay an extra premium and may have to provide a medical certificate to change over from group to individual health insurance. Please note that this process is not mandatory, and it is the insurance companys decision to offer the conversion or not.
Duration Of Cobra Benefits
For an employee, COBRA coverage lasts for up to 18 months. A spouse or dependent child who becomes eligible for any reason other than the employee’s qualifying event can continue COBRA coverage for up to 36 months. For example, if the employee dies, the spouse can continue coverage for 36 months.
Different rules apply in some circumstances. For example, if a spouse is receiving COBRA coverage because the employee was laid off, both the employee and spouse would be entitled to receive benefits for 18 months. However, if the employee dies during this 18-month period, the spouse’s eligibility would be extended to 36 months. COBRA coverage can also be extended if the person receiving benefits has a disability and meets other requirements.
Read Also: What To Do If Health Insurance Claim Is Denied
More Answers: If You Lose Job
- Can a Marketplace plan start the same day I lose my job-based insurance?
-
No. Marketplace plans take effect the first day of the month after your job-based insurance ends. So if you lose your insurance plan on March 7 and select a Marketplace plan by March 31, coverage can start April 1.
- Do I need to provide proof that I lost insurance through my job?
-
You may be asked to provide proof that you lost insurance through your job. Your eligibility notice will explain how to verify your loss of coverage. The Marketplace may also contact you directly.
- When I apply for a Marketplace plan after losing job-based insurance, does the income I made this year before I left my job count?
-
Yes. Savings on a Marketplace plan are based on your estimate of income for everyone in your tax household for the full calendar year you want coverage. Learn how to estimate your yearly income.
- What if I lost my job-based insurance and Im now eligible to enroll in a spouses plan? Can I buy a Marketplace plan instead?
-
Yes. But if youre offered coverage through your spouses job, you arent eligible for premium tax credits or other savings on a Marketplace plan even if you dont accept the offer.
- The only exception is if your spouses plan doesnt meet certain standards for affordability or coverage. Most plans meet these standards, even if they charge high premiums for spouse and dependent coverage.
Can I Get Health Insurance After Quitting A Job
Yes, you can still get health insurance if you quit your job. You can keep your job-based coverage for up to 18 months with a COBRA plan. Or you can buy an individual plan through the Health Insurance Marketplace.
If you have previously paid into a Health Savings Account , the funds are still available to you even if youve left your job. You can use this money to help pay for eligible medical expenses, which can also help to lower health care costs while out of work.
Having health insurance between jobs can help protect you from unexpected out-of-pocket expenses, especially if you were to have a medical emergency while out of work. Either a COBRA plan or an individual plan could be right for you.
You May Like: What Is The Fee For Not Having Health Insurance
