Insurance For Varicose Veins
If you have avoided getting treatment for fear of cost, you dont need to worry. When performed for medical reasons, varicose vein treatment is covered by many insurance companies like BlueCross BlueShied, Cigna, Aetna, United Healthcare and even Medicare. The removal of spider veins, usually done for cosmetic reasons, is not generally covered by insurance, however if they are resulting from an underlying vein disease, some insurance carriers will cover treatment.
Does Medicare Cover Varicose Vein Surgery
There are different types of surgeries for varicose veins the cost changes depending on the type and where you undergo the procedure. For example, vein stripping surgery prices are between $1,500 and $3,000 not including the facility fees. Additional facility or surgery center costs may increase the total amount.
Another varicose vein surgery is called ambulatory phlebectomy. Ambulatory phlebectomy is a much less invasive procedure compared to vein stripping and ligation. Prices change depending on how extensive the service is.
Get A Free Quote
Find the most affordable Medicare Plan in your area
The medical world has several available surgery options for treating varicose veins. Your doctor should discuss your condition and what surgeries may be best for you. Regardless of the surgery you and your doctor decide is best, youll have to pay 20% out of pocket if you dont have supplemental insurance.
How Much Does It Cost To Take Care Of Varicose Veins
The cost of varicose vein treatment depends on several factors, such as whether you have underlying chronic venous insufficiency, the number or size of varicose veins, the chosen treatment plan, anesthesia costs, and whether youre eligible for insurance coverage. Our vein treatment clinics in Long Island provide a complete overview of your varicose vein treatment costs, with and without insurance coverage, before your procedure. As such, you can proceed with your vein treatment with complete mental clarity.
Don’t Miss: How To Get Health Insurance When Unemployed
How Do Health Insurance Companies Define A Medical Necessity
Lets start with what we know. Medical insurance will cover treatment of varicose veins when its a medical necessity. But heres the catch. What one company considers a medical necessity, the next company may not.
Visit our web page on Varicose Veins to learn more. There we discuss the symptoms and treatments of varicose veins. You will learn the specific symptoms that usually make treatment a medical necessity.
The criteria most insurance companies base their coverage approval on are:
1. Annoying or Painful Symptoms
2. Identified Venous Reflux Insurance companies want proof that a vein is not functioning. Documented venous reflux, when blood flows backwards in a vein, is cause for treatment. We diagnose it with ultrasound. However, ultrasound cannot show venous reflux in spider veins they are too small. So, medical insurance doesnt cover the treatment of spider veins. They may make an exception for bleeding spider veins.
3. A specified Time of Unsuccessful Conservative Treatment Did you try an improved diet and exercise plan? Did you wear compression socks daily? Did you rest and elevate your legs each day? The insurance company will want to know this information. Each insurance company has their own requirements. Some insurance companies want you to wear compression socks for 12 weeks.
When Are Treatments Considered Cosmetic
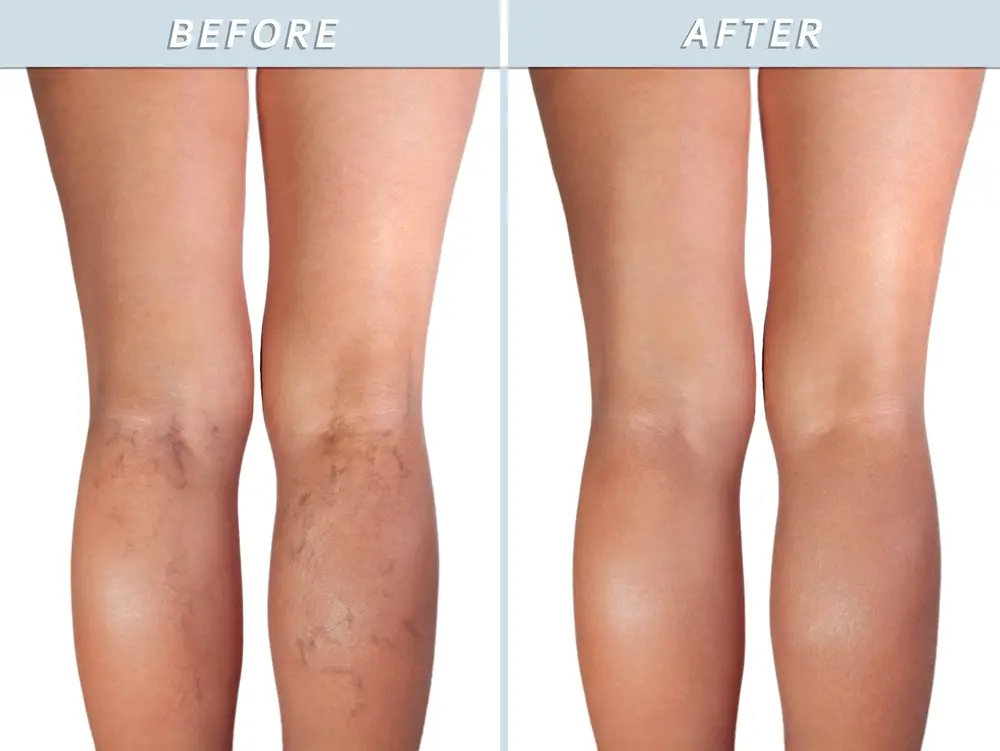
Vein treatments are considered cosmetic when they are performed to address concerns related to your appearance or aesthetic goals. These procedures are not medically necessary but may be performed to address emotional concerns, such as self-consciousness or lack of confidence. However, since the treatment is not a medical requirement, the procedure will be considered cosmetic and will most likely not be covered by your health insurance provider.
Also Check: What Percent Of Health Insurance Is Paid By Employers
Getting Insurance Approval For Varicose Vein Treatment
If you have varicose veins symptoms, your insurance company will require that you have a diagnostic ultrasound. Insurance companies generally cover patients who receive abnormal results from the ultrasound. Still, your insurance company might make you undergo a conservative treatment, such as wearing compression stockings, first. Then, if you still have symptoms and depending on what is required, the insurance company will cover treatments such as radiofrequency ablation , endovenous laser ablation , Venaseal, and Sclerotherapy.
Are Spider Vein Treatments Covered By Insurance
The insurance coverage of spider veins, also called telangiectasia, is slightly more complicated. In many cases, spider veins are considered a cosmetic issue and are typically not covered by insurance. However, they should not be dismissed as merely an aesthetic problem. Spider veins can sometimes develop as a result of an underlying condition, such as venous insufficiency. In such cases, most insurance providers will cover the cost of your procedure, as it will likely be determined medically necessary for your health. If you have noticed the development of spider veins on your face or legs, it is crucial to undergo a vein examination to check whether medical treatment is required and ensure there is no further risk posed to your health.
Recommended Reading: What Is An Average Health Insurance Deductible
Will Insurance Cover Vein Ablations
The typical procedure for removing varicose veins is ablation . For insurance to cover these procedures, they usually require an authorization. Insurance companies have different requirements to grant an authorization, but they typically require that your specialist documents the following:
- Failure of conservative therapy using compression stockings
- A minimum size of the veins along with an ultrasound study and report
- Failure of pain treatment with non-prescription drugs
Our office makes sure this documentation is covered and processes the authorizations. Once you have authorization, your procedure should be covered. Again, its important to check with your insurance company about what you owe for deductibles, co-pays, co-insurance, etc.
Varicose Vein Treatment Costs
Our Patient Choice Advocacy Program at Advanced Vein Institute of Arizona is designed to cover your medical treatments using your health insurance benefits while limiting your out-of-pocket expense. We practice medicine based on our belief in maintaining the highest level of patient care, not based on insurance company guidelines. We are a contracted provider with many health insurance plans to minimize your out-of-pocket expense.
Dont avoid seeking varicose vein treatment because you feel it will be cost prohibitive. In fact, Advanced Vein Institute of Arizona currently offers a free vein screening because we are so confident in our ability to provide superior care in treating your varicose veins.
Don’t Miss: Which Health Insurance Company Is The Best For Medicaid
Does Blue Cross Blue Shield Cover Varicose Vein Treatment
Blue Cross Blue Shield may cover your varicose vein treatment if your situation meets their definition of medical necessity. They provide different levels of coverage for different procedures. Please request free insurance verification to determine if youre eligible for insurance coverage under BCBS.
What Does Medically Necessary Mean
Medicare patients must undergo six weeks of conservative treatment before interventional treatment is covered. Conservative treatment includes weight reduction, daily exercise, compression stockings and periodic leg elevation.
Medicare will deem interventional varicose vein treatment medically necessary if patients still have symptoms of significantly diseased blood vessels after conservative treatment. Some symptoms are pain and edema that interferes with activities of daily living, bleeding, lower leg ulcers, inflammation and clotting in veins near the skins surface.
Additional criteria and limitations apply to certain types of treatment.
Private health insurance companies and plans may have different criteria for covering varicose vein treatments. A Patient Financial Services representative can review these criteria with you.
Recommended Reading: Does Golden Rule Insurance Cover Mental Health
Diagnosis Of Varicose Veins
Your GP will usually be able to tell if you have varicose veins from asking about your symptoms and examining you. They may want to look at your legs both while youre sitting down, as well as while youre standing up. They may also ask you about your medical history.
If your varicose veins are causing symptoms or you have complications, such as bleeding or skin changes, your GP may refer you to a vascular surgeon for assessment and treatment. A vascular surgeon is a doctor who specialises in conditions affecting your blood vessels.
If youre referred, as well as examining you, your doctor may suggest that you have a special type of ultrasound scan called a duplex ultrasound. This uses sound waves to produce an image of the veins inside your leg and the flow of blood through them. It allows your doctor to see your deep veins in more detail, and find out more about the position and extent of your varicose veins.
How To Get Help Paying For Varicose Vein Treatments With Medicare
Medicare may cover your varicose vein removal or treatment. Although you may still have out-of-pocket expenses, including deductibles, coinsurance, and copayment costs. Depending on the treatment type and how often you must go some require more than one session these costs can add up. Thats why having a Medicare Supplement is so important.
Get A Free Quote
Find the most affordable Medicare Plan in your area
Medigap helps to pay for the gaps left by Medicare. Give us a call at the number listed and talk to one of our agents about the best policy for you. Our team of experts can help you find the most suitable options. We compare rates and plans in your area at no cost to you. Cant call? Fill out the online rate comparison form and get the process going now!
- Was this article helpful ?
Read Also: Does The Va Provide Health Insurance
Causes Of Varicose Veins
Varicose veins can develop when valves in your veins dont work properly. Its not clear exactly why this happens. But there are certain factors that seem to put you at greater risk. These include:
- having a family history of varicose veins
- being a woman
- getting older
- being very overweight or obese
Varicose veins may also be secondary to other problems or circumstances. You may get varicose veins if:
- youve had damage to leg veins or a blood clot in the past
- you stand for long periods of time in one position, for example you stand all day at work
- youre pregnant
If you get varicose veins during pregnancy, the good news is that they often improve after your baby is born.
Does Insurance Cover Varicose Vein Treatments San
Health insurance is complicated. When it comes to vein treatment, it can be even more complicated. The good news is varicose veins are not just cosmetic. They
Are varicose veins covered by insurance? The answer is YES, varicose vein treatment is covered by most commercial insurance carriers such as Blue Cross Blue
Also Check: When Does New Health Insurance Start
Can You Reverse Varicose Veins Naturally
No. You cannot reverse varicose veins naturally because theyre symptoms of chronic venous insufficiency, which, in turn, is caused by collapsed or malfunctioning vein valves. Natural remedies cant fix your damaged vein valves. As such, you need to opt for minimally invasive varicose vein treatments to destroy or close the diseased saphenous vein responsible for your vein problems, thereby restoring effective blood circulation to the heart.
Does Health Insurance Cover The Treatment Of Leg Vein Disease
That is a complicated question that cannot be easily answered with a straight Yes or No. It is typically a maybe. But in order to help you understand the process of health insurance coverage and vein disease, we will spend some time explaining the current status of most healthcare insurance plans.
Also Check: How Much Is Health Insurance When You Retire
Ama Disclaimer Of Warranties And Liabilities
CPT is provided “as is” without warranty of any kind, either expressed or implied, including but not limited to, the implied warranties of merchantability and fitness for a particular purpose. AMA warrants that due to the nature of CPT, it does not manipulate or process dates, therefore there is no Year 2000 issue with CPT. AMA disclaims responsibility for any errors in CPT that may arise as a result of CPT being used in conjunction with any software and/or hardware system that is not Year 2000 compliant. No fee schedules, basic unit, relative values or related listings are included in CPT. The AMA does not directly or indirectly practice medicine or dispense medical services. The responsibility for the content of this file/product is with CMS and no endorsement by the AMA is intended or implied. The AMA disclaims responsibility for any consequences or liability attributable to or related to any use, non-use, or interpretation of information contained or not contained in this file/product. This Agreement will terminate upon notice if you violate its terms. The AMA is a third party beneficiary to this Agreement.
Does Insurance Cover Vein Treatment Heart & Vascular Care
Mar 21, 2019 The only way to accurately diagnose your venous disease and to decide whether any procedures are likely to be covered by insurance is to have a
Fortunately, most insurance companies cover varicose vein treatment on symptomatic varicose veins. Learn about the criteria of common insurance companies.
Apr 19, 2019 Varicose Veins are often dismissed as a cosmetic issue, when in fact, they can threaten your circulatory health. Fortunately, many insurance
Don’t Miss: Can I Buy Health Insurance After An Accident
Does Health Insurance Cover Varicose Vein Treatments
Ask your vein specialist about insurance coverage and payment options during your first consultation. You may be surprised to find that your insurance covers many varicose vein treatment procedures when deemed “medically necessary.” Additionally, most vein clinics will offer you a variety of payment methods for those treatments that insurance doesn’t cover.
For a general guideline as to what varicose vein treatments you can expect your insurance to pay for, read on.
American Hospital Association Disclaimer
The American Hospital Association has not reviewed, and is not responsible for, the completeness or accuracy of any information contained in this material, nor was the AHA or any of its affiliates, involved in the preparation of this material, or the analysis of information provided in the material. The views and/or positions presented in the material do not necessarily represent the views of the AHA. CMS and its products and services are not endorsed by the AHA or any of its affiliates.
You May Like: Does My Health Insurance Cover Weight Loss Surgery
What Insurance Do Austin Vein Specialists Accept
We accept all major insurance plans, including Blue Cross Blue Shield, United, Cigna, Humana, Aetna, Ascension Seton Health Plans, Baylor Scott & White, and Tricare, among others. We also accept Medicare. We will work with your health insurance company to get your vein treatments covered whenever possible.
Does Medicare Cover Varicose Vein Removal
The amount you pay for varicose vein removal varies on a large scale. Removal prices include doctors fees, anesthesia, facility cost, meds, and testing. Medical tests like ultrasounds tests can help your provider see your circulation within your veins.
The cost of removal may vary depending on how many sessions you undergo and the method of extraction. Part B will cover 80% of the cost. Again, leaving you with 20% coinsurance unless you have supplemental insurance.
Also Check: Does Health Insurance Include Dental And Vision
Does Medicare Cover Venous Insufficiency
If you have venous insufficiency, that means your veins struggle to send blood from the legs back up to your heart. Without treatment, this may weaken the vein walls and damage your valves. Medicare covers venous insufficiency if lifestyle changes dont help.
Part D may include some of the medications your doctor prescribes. Check your plans formulary to make sure your prescription is on their list of covered drugs. Otherwise, ask your doctor for an alternative that your policy does cover.
When Vein Removal Is Medically Necessary
Swollen and painful veins are considered symptomatic of medically necessary treatment. While you can encourage blood flow around the affected area by wearing thigh-high compression stockings, varicose veins will remain until they are surgically removed or closed.
Most insurance companies will ask to review the results of a venous ultrasound before providing coverage for varicose vein treatments. Conducted in a vein specialists office, a short consultation appointment is covered under most insurance plans, and the provider will be able to present the quality of your veins. If the ultrasound produces findings that your varicose veins are causing swelling, ulcers, heaviness, or backward blood flow, your treatment will be labeled as medically necessary. This evidence will provide your insurer with what they need to cover the removal procedure.
Read Also: What’s The Average Deductible For Health Insurance
Are Varicose Veins Just A Cosmetic Issue
No. Varicose veins signal that the valves in the leg are weak or damaged which affects circulation and can cause aching pain and discomfort. Sometimes, varicose veins can lead to more serious medical problems, such as ulcers and bleeding. Painful varicose veins, ulcers or blood clots often require surgery, plus lifestyle changes.
I Have Had A Blood Clot Before And I Am Worried
I am scheduled for a right leg radiofrequency ablation. I have venous insufficiency in the saphenous vein and have had a blood clot before. Question: In 2006, I underwent an artificial lumbar disk implant. This failed causing artificial disk to move into the spine. While surgeon removed the artificial disk implant, he nicked the liac
Recommended Reading: How Do Self Employed People Get Health Insurance
Does Health Insurance Cover Varicose Vein Treatment
Most health insurance will cover treatment of chronic venous insufficiency the condition that is often responsible for varicose veins. If varicose veins are painful, interfere with daily activities, and are caused by CVI, its likely your insurance plan will cover at least some of your treatment, depending on your deductible and other factors.
As with any medical treatment, insurance policies differ, and its best to ask about coverage beforehand. Your doctor can provide the necessary information for you to check with insurance before obtaining any treatment.
Definition of Medically Necessary Treatment
With varicose veins , poorly functioning valves allow the blood to pool in the lower leg and cause symptoms. Varicose veins can occur in almost anyone, affecting up to 35% of Americans.
Varicose veins can cause symptoms including discomfort and bleeding when a vein bursts as a result of minor trauma. Most insurance policies recognize that venous insufficiency is a real disease and treatment isnt merely cosmetic.
Most insurance companies require that the varicose veins cause leg pain or other symptoms that affect daily life. If you have to stand to do your job, for example, varicose veins can prevent you from working or require frequent breaks to elevate your legs. An inability to do housework or exercise can also negatively impact daily life.
Weve provided a list of questions to ask your insurance provider to find out if your treatment will be covered.
