How Medicaid Works With Private Insurance
If you are already enrolled in private health insurance, Medicaid benefits are applied a little differently. While each state has its policies and eligibility requirements associated with Medicaid, individuals struggling to pay premiums can often combine their existing health insurance plan with Medicaid.
Once you have had a visit with your doctor or hospital, the benefits departments coordination determines which of your health insurance plans will be billed for the services. Typically, Medicaid is only charged once the coverage from the private insurer has reached its limits.
Medicaid will then allocate money towards the premium payment and disperse these funds to the individual each month in a check. Listing Medicaid as your primary health insurance provider while also being enrolled in a private health insurance plan will often delay billing. It can cause other issues that can delay benefits. Because Medicaid always is the second-payer option, listing it as such will ensure bills are sent to the correct spot and benefits continue as usual. More information can be found here: Coordination of Benefits & Third Party Liability | Medicaid
How Are My Health Care Costs Reimbursed If I Have Medicare And Medicaid
When dual eligible beneficiaries have healthcare expenses, Medicare pays first and Medicaid pays last. But this is not the case for things Medicare doesnt cover, like long-term care. If Medicaid is covering a beneficiarys long-term care, Medicare will still be the primary payer for any Medicare-covered services like skilled nursing care or physical therapy.
Although it is less common, if a dual eligible individual has additional coverage then Medicare pays first, Medigap will pay second, and Medicaid is the last payer for their claims .
Health Insurance Premium Payment
The Health Insurance Premium Payment program is a Medicaid program that helps families pay for private health insurance. This program is for families who have:
- A parent or a spouse with private health insurance
- A child or a spouse with Medicaid
Medicaid will pay the family’s private health insurance if the total cost of that insurance is less than the total cost of care with Medicaid. The total cost of the private insurance includes the premium, coinsurance and deductibles.
If approved, Medicaid may pay the private health insurance costs for the entire family and not just for the family members who get Medicaid. The family will get services through the private health insurance plan.
To learn more or to apply, visit the Get HIPP Texas website or call us toll-free at 800-440-0493. You also can ask us to send you an application. Write to:
Texas Health and Human Services CommissionTMHP-HIPP
Also Check: Where To Shop For Health Insurance
Unitedhealthcare Senior Care Options Plan
UnitedHealthcare SCO is a Coordinated Care plan with a Medicare contract and a contract with the Commonwealth of Massachusetts Medicaid program. Enrollment in the plan depends on the plans contract renewal with Medicare. This plan is a voluntary program that is available to anyone 65 and older who qualifies for MassHealth Standard and Original Medicare. If you have MassHealth Standard, but you do not qualify for Original Medicare, you may still be eligible to enroll in our MassHealth Senior Care Option plan and receive all of your MassHealth benefits through our SCO program.
Medicaid Is Structured As A Federal
Subject to federal standards, states administer Medicaid programs and have flexibility to determine covered populations, covered services, health care delivery models, and methods for paying physicians and hospitals. States can also obtain Section 1115 waivers to test and implement approaches that differ from what is required by federal statute but that the Secretary of HHS determines advance program objectives. Because of this flexibility, there is significant variation across state Medicaid programs.
The Medicaid entitlement is based on two guarantees: first, all Americans who meet Medicaid eligibility requirements are guaranteed coverage, and second, states are guaranteed federal matching dollars without a cap for qualified services provided to eligible enrollees. The match rate for most Medicaid enrollees is determined by a formula in the law that provides a match of at least 50% and provides a higher federal match rate for poorer states .
Figure 2: The basic foundations of Medicaid are related to the entitlement and the federal-state partnership.
Read Also: How Can A College Student Get Health Insurance
If You Decide To Pay Full Price For A Marketplace Plan
You can have both a Marketplace plan and Medicaid or CHIP, but youre not eligible to receive advance payments of the premium tax credit or other cost savings to help pay for your share of the Marketplace plan premium and covered services. If you or others on your Marketplace application choose to have Medicaid or CHIP and full-price Marketplace coverage:
- End your Marketplace plan with premium tax credits if youre the only one on the application.
- Submit a new application for Marketplace coverage without premium tax credits or other cost savings. Note: You can only enroll in Marketplace coverage during the annual Open Enrollment Period or if you qualify for a Special Enrollment Period.
- Notify your state Medicaid or CHIP agency of your Marketplace enrollment. Note: You may no longer be eligible for CHIP.
Can I Apply For Medicaid If We Already Have Private Health Insurance
Medicaid is one of the most famous entitlement programs in America, but there is some confusion on who can apply and how they can do it. Medicaid is available to people who fit into several categories, including those with very low incomes, some who are disabled and the children of people who fit into various categories. If youre thinking about trying to qualify for Medicaid, you need to know whether you qualify. One of the most common questions has to do with private health insurance. Are you barred from seeking Medicaid if you already have insurance? The short answer is no, but there are other questions to answer about your financial situation.
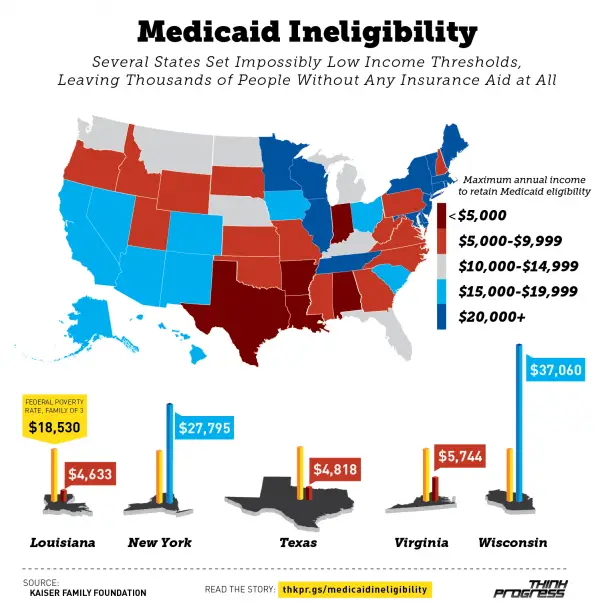
Medicaid eligibility varies from state to stateThe first thing to know about Medicaid eligibility is that there is no singular national standard. The original version of the Affordable Care Act sought to force states to expand Medicaid to include people up to a higher level of income. The Supreme Court struck this down as unconstitutional, though, leaving states to make a choice on expansion. While some states chose to expand the program, others chose to keep it the same. This has let to a hodgepodge of state requirements.
You May Like: Where Can I Go For Health Care Without Insurance
Assistance Programs For Pregnant Women
Wyoming provides assistance to eligible women during pregnancy to provide a safe and healthy experience for the mother and giving the baby the best possible beginning to life.
Presumptive Eligibility For Pregnant Women
Presumptive Eligibility for Pregnant Women is a Medicaid option designed to improve an applicants access to temporary Medicaid while their eligibility for full Medicaid benefits is being determined. Eligible pregnant women are limited to outpatient services through a Medicaid provider for up to 60 days after completing an application for Medicaid.
To qualify a woman must be:
- Pregnant
- Income eligible at or below 154% of the Federal Poverty Level.
To apply visit your local Public Health Nursing office.
Pregnant Women
Wyoming Medicaids Pregnant Women programs provide health coverage for eligible pregnant women for up to 60 days post-partum. Pregnant women with income below the family care income guidelines must cooperate with Child Support Enforcement once the baby is born to continue eligibility.
To be eligible a woman must be:
- Pregnant
- Income eligible at or below 154% of the FPL
- A U.S. citizen or lawfully present in the U.S
- A Wyoming resident.
Pregnant By Choice
The Pregnant by Choice program provides pregnancy planning services to women who have received Medicaid benefits through the Pregnant Women program.
To be eligible a woman must be:
- In the 60 days post-partum period and on Wyoming Medicaids Pregnant Women program
Parents and Caretaker Relative
Who Is Eligible For Medicaid
You may qualify for free or low-cost care through Medicaid based on income and family size.
In all states, Medicaid provides health coverage for some low-income people, families and children, pregnant women, the elderly, and people with disabilities. In some states the program covers all low-income adults below a certain income level.
- First, find out if your state is expanding Medicaid and learn what that means for you.
- If your state is expanding Medicaid, use this chart to see what you may qualify for based on your income and family size.
Even if you were told you didn’t qualify for Medicaid in the past, you may qualify under the new rules. You can see if you qualify for Medicaid 2 ways:
- Visit your state’s Medicaid website. Use the drop-down menu at the top of this page to pick your state. You can apply right now and find out if you qualify. If you qualify, coverage can begin immediately.
- Fill out an application in the Health Insurance Marketplace. When you finish the application, we’ll tell you which programs you and your family qualify for. If it looks like anyone is eligible for Medicaid and/or CHIP, we’ll let the state agency know so you can enroll.
Read Also: What Is My Health Insurance Plan
What Services Does Medicaid Cover
Medicaid covers more than 60 percent of all nursing home residents and roughly 50 percent of costs for long-term care services and supports.
Federal rules require state Medicaid programs to cover certain mandatory services, such as hospital and physician care, laboratory and X-ray services, home health services, and nursing facility services for adults. States are also required to provide a more comprehensive set of services, known as the Early and Periodic Screening, Diagnostic, and Treatment benefit, for children under age 21.
States can and all do cover certain additional services as well. All states cover prescription drugs, and most cover other common optional benefits include dental care, vision services, hearing aids, and personal care services for frail seniors and people with disabilities. These services, though considered optional because states are not required to provide them, are critical to meeting the health needs of Medicaid beneficiaries.
About three-quarters of all Medicaid spending on services pays for acute-care services such as hospital care, physician services, and prescription drugs the rest pays for nursing home and other long-term care services and supports. Medicaid covers more than 60 percent of all nursing home residents and roughly 50 percent of costs for long-term care services and supports.
How Much Does Medicaid Cost? How Is It Financed?
Can I Get Medicaid And Medicare At The Same Time
You may in some situations. Medicare is a health insurance program for:
- People ages 65 and older
- People younger than age 65 who are disabled
- People with end-stage kidney disease
With Medicare, you have to pay monthly premiums and other costs, such as copays and deductibles, when you go for medical care. If you are on Medicare and have a limited income, you may qualify for help from Medicaid to pay the costs of Medicare. If you have both Medicaid and Medicare, you may hear people refer to you as being dually eligible.
Read Also: Is It Required By Law To Have Health Insurance
How To Use Your New Medicaid And Chip Coverage
- Category:Health Insurance
Now that you have joined the millions of citizens registered in Medicaid or CHIP coverage, its critical to use your new health insurance plan.
If you have concerns, you should contact your states insurance company. When you visit health government online portals, scroll down and choose your country from the menu at the bottom of these pages.
What Is Nevada Check Up

Nevada Check Up is the State of Nevadas Childrens Health Insurance Program . Depending on your income, your children may qualify for coverage through Nevada Check Up. If you qualify, you will be required to pay a quarterly premium based upon your family size and income, but wont be responsible for things like co-payments and deductibles.
In Nevada, children living in households with an annual income of up to 200% of the federal poverty level may qualify for coverage through Nevada Check Up. This is $50,200 for a family of four.
Recommended Reading: Do Employers Pay For Health Insurance
Medicaid As Secondary Insurance
Can you use Medicaid as a secondary insurance? If you take your employers insurance or you have private coverage, you might still have trouble paying deductibles and co-pays. But qualified low-income families and individuals might be able to cover co-pays, deductibles, and insurance premiums by using Medicaid as a secondary insurance.
Just keep in mind that Medicaid is always the last resort payer if you have coverage through another agency. Secondary payers usually cover the smaller amount, like coinsurance or co-pay, while primary insurance covers the bigger costs.
Does Medicaid Cover Hot Tubs
In most states, yes. Thats assuming that the hot tub is prescribed as a necessary piece of durable medical equipment by your doctor. And it doesnt mean your insurer will make the process easy.
Some states have restrictions on qualifying DME, though restrictive policies can in some cases be litigated.
Read Also: How To Stop Health Insurance
Texas Medicaid Wellness Program
The Texas Medicaid Wellness Program is a special health program for people who get Medicaid and have long-lasting or serious health conditions. These conditions can include asthma, diabetes, congestive heart failure, coronary artery disease, chronic obstructive pulmonary disease , and others.
People in this program can get help any time of day or night with:
- Getting an answer to a health question.
- Finding a main doctor.
- Managing their health between doctor visits.
- Learning more about their health conditions.
- Knowing how to take their medicines.
- Picking the best medical care for their health.
Learn more about the Wellness Program.
Are Massages Covered By Health Insurance
Are you in desperate need of a massage?
Well, you may be able to get that covered, too. Especially if you have chronic back pain, were in an accident, or see a chiropractor/physical therapist regularly. If you have pain, talk to your physician about it. If you can get a prescription from any of these medical specialists for massages, insurers will often cover the therapy.
Dont know where to find a masseuse in your area? Use Spafinder Wellness 365s search tool.
Recommended Reading: How Much To Employers Pay For Health Insurance
How Do You Get Health Insurance If You Dont Qualify For Medicaid
Every state has different criterias to find out who qualifies for Medicaid. You may be qualified for Medicaid if:
- Youre handicapped.
- Rhode Island
- District of Columbia
Although there is no penalty for being uninsured, it is still advised that people have some sort of health coverage. Healthcare costs in America are constantly rising. Therefore, it is better to have an insurance plan that keeps you covered in times of need. If you unfortunately have to go to the hospital for an emergency, need to have a surgery, or face a severe accident, you will end up in the hospital. You do not want to be handed a hospital bill of worth thousands of dollars now, do you? Therefore, having health insurance will provide coverage in dire situations and you wont have to worry about huge hospital bills.
Are There Special Medicaid Programs For Women
Yes, if you have been diagnosed with breast or cervical cancer through a state screening program and you have a low income. You can get medical treatment through your state’s Breast and Cervical Cancer Prevention and Treatment Program.
Most states will cover pregnant women and may allow you to get Medicaid, even if you have a higher income than what is required to be eligible for the program.
Also Check: How Much Does Usps Health Insurance Cost
Are You Looking For Free Insurance Quotes
Secured with SHA-256 Encryption
|
D. Gilson is a writer and author of essays, poetry, and scholarship that explore the relationship between popular culture, literature, sexuality, and memoir. His latest book is Jesus Freak, with Will Stockton, part of Bloomsburys 33 1/3 Series. His other books include I Will Say This Exactly One Time and Crush. His first chapbook, Catch & Release, won the 2012 Robin Becker Prize from Seve… |
- The majority of clinics accept Medicare
- This can also apply to a variety of specialty providers like eye doctors and dentists
- For a standard doctor visit, you can expect to pay 20% of the approved Medicare cost
With the Medicare health insurance plan, youll have all of your medical needs taken care of at an affordable price. The number of clinics that accept Medicare will likely be greater than you expect, so its important to compare providers before you go.
While youre researching quotes for clinics that accept Medicare, enter your ZIP code into our free quote tool above to compare quotes from Medicare insurance companies near you.
- Speech-language therapists
- Psychologists and psychiatrists
With these providers, you can take care of your mental, muscular, and vocal needs to ensure that youre in the best shape that you can be.
The cost isnt too high either, as most patients can see their doctor and only have to pay 20% of the cost of the Medicare-approved amount.
Middle Class Cant Afford Health Insurance
The Affordable Care Act has stretched out wellbeing inclusion to more than 20 million individuals and has brought down the expense of inclusion or care for millions more. In any case, a successive analysis of the law is that it has not done whats needed to make inclusion moderate for center pay singular market shoppers. The answer for this issue is clear. Expanding or disposing of the salary top on the ACAs exceptional tax breaks would guarantee that practically all purchasers have inclusion alternatives that cost under 10% of their earnings.
Don’t Miss: What Is The Best Health Insurance In Alabama
