Assessing The Tax Penalty
Beginning in 2014, you are assessed a tax penalty for failing to cover yourself under a health insurance premium. In 2014, the penalty was $95 per person. In 2015, it increased to $325 in 2016, to $695 per adult. Beginning in 2017, the amount is the same as 2016 but adjusted for inflation and is also based on your income. The adjustment was zero in 2017 and 2018. If you are canceling your health insurance, make sure you have another option in place or face a higher bill at tax time.
References
Can I Cancel Health Insurance After One Month
While you can cancel your private health insurance at any time, you wont be able to select a new health plan outside of the open enrollment period unless you meet certain qualifying reasons. If you miss this 30-day window youll have to wait until your companys open enrollment period comes around again.
Special Enrollment Periods For Health Insurance
Special enrollment periods are so named because thats exactly what they are: special. During a special enrollment period, only you and your family have the chance to decide on new coverage options.
Special enrollment periods are triggered by specific events, including:
- Getting married, divorced or legally separated
- Giving birth or adopting
- Starting, ending or losing a job
- Losing other health insurance coverage
- A death in the family
- Moving to a new ZIP code or county
- Certain other qualifying events
If one of these events applies to you, youll usually have 60 days to switch to a new plan or make changes to your existing one.
Just like with open enrollment, you can shop around and compare plans by talking to your existing health insurance provider, your broker or visiting your states health insurance marketplace. In some cases, youll need to provide evidence of your qualifying life event before enrollment is complete.
Also Check: How To Get Health Insurance Fast
How To Get Out Of Your Employer’s Group Health Plan Mid
Written by: Josh MinerSeptember 15, 2020 at 9:01 AM
Employees have two options for getting out of their employers group health plan mid-year. IRS Notice 2014-55 outlines two ways employees covered by their employers health plan can change their health insurance plan elections during a plan year. Heres what you need to know about the rules:
Can Employers Cancel Benefits Due To Financial Burden
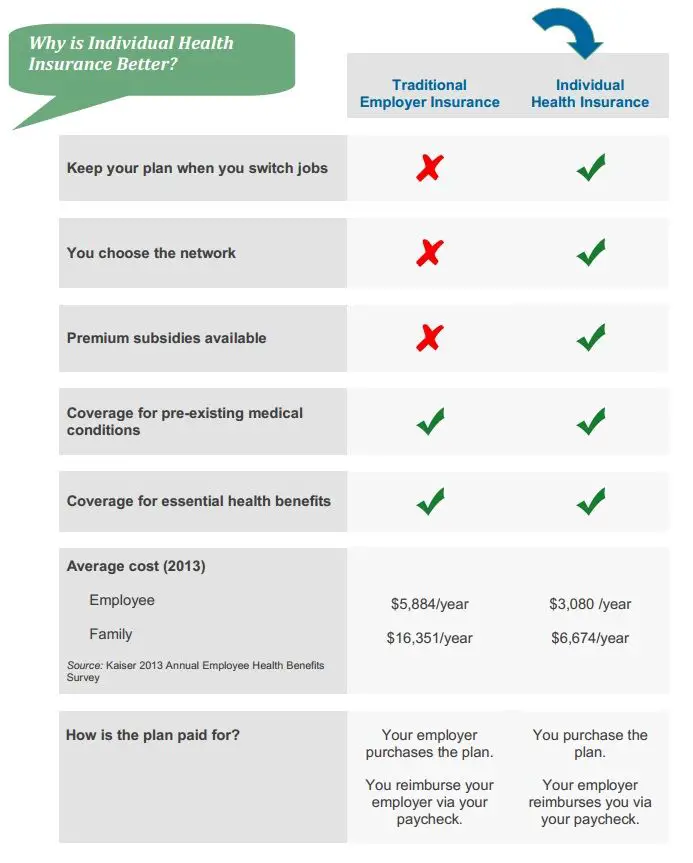
Another worry that some employees have is that their employer will cancel their insurance if their health issues have become a financial burden. However, an employer cant cancel an employees benefits simply because their medical care is expensive.
The same goes if youve become disabled. The Affordable Care Act prohibits an employers insurance provider from canceling a persons health insurance just because theyve developed a disability.
Read Also: Does Amazon Have Health Insurance
Changing Your Health Insurance: Why You Might Want To
People choose to change their health insurance plans for all kinds of reasons. A few of the most common include:
- Changes in your plans network If your preferred doctors or specialists stop accepting your insurance, you could pay significantly more. Other health insurance options may help lower your overall medical bills.
- Needing more or less coverage If, for example, you visit the doctor frequently and copays are eating into your budget, a different plan may help you keep medical expenses under control. On the other hand, if youre paying for top-tier coverage but dont often use it, a more modest plan could be a better fit.
- Moving, changes to your employment or changes to your family These events are often times when its important to review your entire financial situation. Along the same lines, theyre also times when youll be able to switch your health insurance coverage.
No matter why you want to switch health insurance plans, there are two windows of opportunity when you can: annual open enrollment and special enrollment periods.
Gaining Access To A Qsehra Or Individual Coverage Hra
This is a new special enrollment period that became available in 2020, under the terms of the Trump Administrationss new rules for health reimbursement arrangements that reimburse employees for individual market coverage. QSEHRAs became available in 2017 and allow small employers to reimburse employees for the cost of individual market coverage . But prior to 2020, there was no special enrollment period for people who gained access to a QSEHRA.
As of 2020, the Trump administrations new guidelines allow employers of any size to reimburse employees for the cost of individual market coverage. And the new rules also add a special enrollment period listed at 45 CFR 155.420 for people who become eligible for a QSEHRA benefit or an Individual Coverage HRA benefit.
This includes people who are newly eligible for the benefit, as well as people who were offered the option in prior years but either didnt take it or took it temporarily. In other words, anyone who is transitioning to QSEHRA or Individual Coverage HRA benefits regardless of their prior coverage has access to a special enrollment period during which they can select an individual market plan , on-exchange or outside the exchange.
This special enrollment period is available starting 60 days before the QSEHRA or Individual Coverage HRA benefit takes effect, in order to allow people time to enroll in an individual market plan that will be effective on the day that the QSEHRA or Individual Coverage HRA takes effect.
Also Check: Do You Have Health Insurance
What If I Want To Change My Insurance Company Or Coverage
One of the requirements for that pre-tax status is that once you have made your coverage choices, changes can be made only within 30 days of a qualifying event, or during the next open enrollment period. The open enrollment period can be any time of year and is generally tied to the renewal of the policy. The most common times for open enrollment is mid-to-late fall or mid-spring .
Qualifying events: A qualifying event for health insurance coverage would be things like when youre hired on, the birth of a child, marriage, etc. Health insurance companies lay these events out for reference as needed. If you have questions regarding why, you can always ask your employer or the insurance company. Sometimes, it comes down to company policy. In general, if you have other coverage or meet certain qualifications, they should allow you to drop their healthcare and avoid deductions from your paycheck.
How To Cancel Your Health Insurance
ACA and private major medical health insurance policies
There are several potential reasons why you may want to cancel your major medical insurance policy.
If youve recently turned 65 and are now Medicare-eligible youll want to cancel your individual major medical policy and transition to Medicare.
Or perhaps you recently got a job with employer-sponsored benefits and need to cancel your ACA or private health insurance policy.
You may be weighing the risks and benefits of keeping your major medical insurance considering that beginning January 1, 2019, the , effectively undoing the ACA .
You may be asking yourself:
- Is it a good idea to cancel your health insurance?
- What are your options for more affordable major medical coverage or non-ACA insurance?
Well explore those questions and explain how to cancel your health insurance in the remainder of this blog post. You can also to get started.
Insurance With Lower Monthly Premiums
Short term health insurance can provide temporary and limited benefits for a lower premium if you qualify. STM is not a replacement for comprehensive major medical coverage.
You May Like: What Is The Self Employed Health Insurance Deduction
Can You Cancel Your Marketplace Insurance At Any Time
Are you wondering as to whether you can cancel your Marketplace insurance at any time or not? If so, then the answer to this question is, yes. You can drop your Marketplace insurance at any given time. You may need to do this on the off chance that you get other wellbeing inclusion, or for another explanation. You can end inclusion for everybody on the application after your inclusion has begun. Your end can produce results when the day you drop, or you can set the Marketplace inclusion end date to a day later like in the event that you realize your new inclusion will begin the main day of the next month. In addition to this, you can even cancel your Marketplace insurance for simply a few people on the application. Most of the time, their inclusion will end right away.
What Is A Special Enrollment Period
Under the Affordable Care Act , a special enrollment period is a set period in which you would be allowed to enroll in or change your health insurance coverage. The special enrollment period lasts 60 days from the date of a qualifying life event. During these 60 days, you would be allowed to enroll in a new health insurance plan.
Once the 60 days have expired, the SEP would be over. At that point, you would have had to submit an application for a new policy to receive coverage. If you did not choose a policy and don’t have existing coverage, then you would have no health insurance or could enroll in state-run programs like Medicaid if you are eligible.
Read Also: Where Can You Get Affordable Health Insurance
Exceptional Cases For Cancelling Health Insurance
- Child Support or Divorce: You might be legally obligated to maintain your health insurance policy as part of court-ordered child support or divorce proceedings. Also, if a Medicare recipient decides to get private insurance or HMO coverage, that person must apply to the Health Care Financing Administration before changing insurers or plans.
- When You Cancel Medicare and Want to Switch to Private Coverage: When someone covered by Medicare decides to switch to better private insurance, say, through coverage offered by a new job, that person must apply to the Healthcare Financing Administration before changing insurers or plans.
What To Know If You’re Replacing Your Policy
Always be clear on why you want to replace your policy and the pros and cons of switching.
If you’re replacing a car or home insurance policy, make sure your new policy provides coverage before the cancellation date of your old policy. If not, you risk not having coverage while waiting for the new policy to take effect.
If you’re replacing a life or health insurance policy, you may be asked for new medical information. You risk no longer being eligible or your premiums increasing if there has been changes in your health.
Read Also: Is Eye Surgery Covered By Health Insurance
Can You Cancel Your Insurance Policy At Any Time
Check for potential penalties If you decide that switching car insurance is the right option, find out if there are any penalties for changing before the end of the coverage period. Fortunately, auto insurance companies generally give you the right to cancel your policy at any time as long as you give proper notice.
How To Cancel Your Private Health Insurance Policy
If you worked with a personal insurance agent to enroll in a plan, contact that individual to begin the cancellation process.
If you purchased a private individual major medical policy directly from an insurance company , these are the steps to take to cancel it:
Review your bill:
Don’t Miss: How To Apply For Low Cost Health Insurance
Newly Qualify For Health First Colorado
If you are enrolled in a health insurance plan through Connect for Health Colorado and later qualify for Health First Colorado , you will still need to call us to request to cancel your plan. This is because you can choose to stay enrolled in the plan. However, you will no longer qualify for financial help to lower the monthly cost.
Why Chooseinsuranceonlinecomcom
You can easily find the latest and accurate insurance information from ChooseinSuranceOnlinecom.com.
Most of the time, you need it to save your time and avoid being deceived!
How? When you are looking for can you cancel your insurance at any time.There are too many fake insurances that have not been verified on the Internet. How long does it take to find a truly reliable official insurance?
But with us, you just type can you cancel your insurance at any time and we have listed all the verified insurance pages with one click button to Access the Page.
Not just for this one, but we have created database of 1,00,000+ insurances and adding 50 more every day!
Don’t Miss: Can A Child Have 2 Health Insurance Plans
How To Prove A Qualifying Event
After applying for marketplace coverage during a special enrollment period, you may need to provide documentation of your qualifying life event so the insurance provider can confirm that you meet SEP requirements.
Once you have selected a health insurance plan, you will have 30 days to send documents to the insurance provider that detail your qualifying life event. It is important to note that your policy will begin when you have picked a plan, but you will not be able to use the insurance until your eligibility has been confirmed and the initial premium has been paid. Furthermore, if you are not approved for an SEP, then the policy will be canceled or you will need to provide additional documents supporting the qualifying event.
For example, if you were recently married and wanted to change your health insurance policy, you would be required to provide documents that specify the names of you and your spouse, along with the date of the marriage. In this case, you would have 60 days from the date of your marriage to select a new health plan and 30 days from the time you choose a plan to submit supporting paperwork. Some acceptable documents you could use would be a marriage certificate or a copy of your marriage license.
How To Make Changes
To make changes, such as enroll a dependent or elect a different health plan, you must complete and submit the required form during the annual open enrollment or when a special open enrollment event occurs, within the timelines listed below.
To make a change during the PEBB Programs annual open enrollment:The PEBB Program must receive the appropriate PEBB Continuation Coverage Election/Change or PEBB Continuation Coverage Election/Change form. You may also make some changes using PEBB My Account.
To make a change when a special open enrollment event occurs:The PEBB Program must receive the appropriate PEBB Continuation Coverage Election/Change or PEBB Continuation Coverage Election/Change form no later than 60 days after the event that created the special open enrollment along with proof of the event that created the special open enrollment . If adding a newborn or newly adopted child, and adding the child increases your premium, your employer must receive this form no later than 60 days after the birth or adoption.
Also, if you or your eligible dependent are interested in enrolling in a PEBB Medicare supplement plan, you have 6 months from the date of your enrollment in Medicare Part B to enroll.
You May Like: How Much Do Health Insurance Agents Make
How Do I Cancel My Health Insurance
In case youre dropping an arrangement that you bought on a medical coverage marketplace, for example, healthcare.gov or a state commercial center, you can drop the strategy by signing into your marketplace account. Once you have signed in, choose the My Plans and Programs options and hit End All Coverage. Set your inclusion end date and adhere to the last directions to drop your approach. You can likewise call the commercial center assistance community on the off chance that you need assistance or are changing to an administration run wellbeing program.
In case youre dropping a secretly bought arrangement, you can call your medical coverage organization straight forwardly. Your insurance providers telephone number ought to be imprinted on your approach, medical coverage card
How To Cancel Medicaid Or Chip Programs

- Income Adjustment: Expect the state to notify you If your household income increases or state qualification standards change, and you, therefore, are no longer eligible for Medicaid or the Childrens Health Insurance Program. If you lose your Medicaid or CHIP coverage, you will have a 60-day special enrollment window to buy a Marketplace plan, assuming you can afford to do that after receiving common government subsidies. Nearly 90% of those with Obamacare get subsidies.
- Notify Your Caseworker: If you must cancel your Medicaid or CHIP plan because you get a new job or your child turns 19 and ages out, you will have to research the process in your state. State rules vary significantly. Start by calling your state Medicaid department caseworker. Typically, you will have up to 30 days to enroll in a Marketplace plan before losing your Medicaid or CHIP coverage.
Recommended Reading: Where To Find Health Insurance
